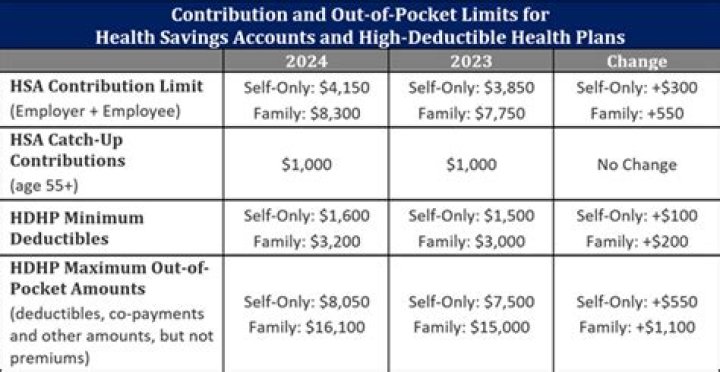
Does Medicare Pay for Assisted Living Expenses? Medicare, which is a type of health insurance that Americans 65 and older are eligible to receive, does not typically cover the expenses associated with assisted, independent or retirement living. Assisted living. Long-term care in a nursing care community.
What is a therapeutic leave of absence?
Therapeutic leave means the resident leaves the facility to go to a family-type setting and not to another nursing facility. One day is defined as an overnight stay away from the nursing facility.
What does therapeutic leave mean?
In states that permit such leave these visits are called “therapeutic leave.” Therapeutic leave is considered a non-medical visit outside the facility most commonly used for overnight visits with family or friends.
What is a therapeutic pass?
2.1. Off-unit Therapeutic Pass – a temporary, time-limited pass that allows a PHF patient to be accompanied off the unit by a staff member for therapeutic, socialization, and/or – community integration purposes only.
How many days will Medicare pay for assisted living?
Medicare will pay for 100% of the cost of care up to 20 days at a skilled nursing facility and approximately 80% of the cost up to 80 more days. The care must be for recovery following an inpatient hospital stay. Medicare does not cover any cost of assisted living.
What are 5 residents rights?
The right to exercise self-determination. The right to exercise freedom of speech and communicate freely. The right to participate in the creation and review of one’s individualized care plan. The right to be fully informed in advance of any changes to care plan or status of the nursing home.
Does Medicare pay for bed hold?
The nursing home is required to tell you in writing of its bed hold policy both at the time of admission and at the time you are transferred to the hospital. Medicaid, Medicare and most private insurers will not pay for a bed hold.
What is a Medicare skip day?
Source: This is from the Medicare SNF Manual (Pub 12} A leave of absence day, also known as a “skip” day, occurs when a patient leaves the facility before midnight, returns within 24 hours, and is not admitted to the hospital as an inpatient.
Can a nursing home bill Medicare for leave of absence?
The Medicare Benefit Policy Manual says that such a notice is “not appropriate.” [3] If the resident begins a leave of absence and returns to the facility by midnight of the same day, the facility can bill Medicare for the day’s stay. [4]
Can a Medicare Part a patient stay in a SNF?
Such a facility is certified as a SNF. Inside the facility, a Medicare patient may use up his Part A eligibility as a SNF patient…but is not strong enough to return home. And so after his Part A eligibility runs out, the patient remains in the facility as a custodial care patient.
Can a person leave a nursing home with Medicaid?
Two of the most common concerns are losing Medicaid or Medicare coverage for their stay and possibly losing their bed in the facility. Can a Resident Leave a Nursing Home? The good news is that nursing home residents are typically permitted to take some time away from their facilities.
What happens when a skilled nursing facility is not covered by Medicare?
A resident whose full stay is not covered (either because the resident has no days left in the benefit period or because the resident needs professional therapy services fewer than five days per week) may qualify for therapy services under Medicare Part B, as an outpatient service.